Below are some of the most common questions we receive from patients who are considering proceeding with a Posterior Lumbar Decompression and Fusion. Please keep in mind that the recovery from surgery is quite subjective and is affected by various factors such as patient age, comorbid illnesses, degree of the spinal cord or nerve impingement, the length of illness prior to surgery as well as a degree of disability prior to surgery to name a few. The answers below are based on the average patient that we see.
What Causes Lower Back Pain?
Lower back pain and pressure is often caused by lumbar spinal stenosis, which is often created by spondylolisthesis, a slippage of a spinal disc, or degenerative changes. When this happens, the disc pushes on nearby nerve roots and causes lower back pain and pain that can radiate down into the legs. Fusion may be needed to stabilize the spine, as the motion and degenerative changes can continue to irritate the nerve roots and continue to cause back and leg pain.
Degenerative disk disease in the lumbar spine can also be the cause of lower back pain and pressure. Because spinal discs do not have a blood supply, if a disc is injured due to wear and tear or a traumatic injury, it cannot repair itself. Degenerative disc disease affects nearly one-third of people between 30 and 50 years of age, although the degeneration may not be bad enough to lead to pain and future fusion surgery. If the outer portion of the disc breaks down, the inner gel-like portion of the disc can leak out and irritate nearby nerves. In some cases, the disc collapses enough to compress a nerve root. If this leads to chronic, debilitating pain, decompression and fusion surgery may be necessary.
What Is Posterior Lumbar Decompression And Fusion (PLDF)?
Posterior lumbar decompression and fusion (PLDF) is a surgical procedure that aims to relieve pain, and pressure on the spinal cord and the nerves in the lower back. The lower back is made up of the lumbar spine, where the spine curves inward toward the abdomen. It consists of the five vertebrae, L1-L5. They end in the sacral region, which connects the lumbar spine with the tailbone.
Because they bear the most weight, the lowest two vertebrae in the lumbar spine, L4 and L5, are most prone to degradation and injury and are the most often fused.
Lumbar Fusion Surgery Benefits
Posterior lumbar decompression and fusion is performed to relieve chronic, debilitating pain and pressure on the spinal cord and the nerves in the lower back. By limiting movement of the vertebrae causing the pain, and by removing disc material and areas of the vertebrae that are impinging on nearby nerves, the pain is usually relieved. For patients who have tried various nonsurgical alternatives and still have chronic pain, this surgery can return quality of life.
How Effective Is Lumbar Spinal Fusion?
Most of our patients experience a significant improvement in back and leg pain within a reasonable amount of time after the spinal decompression procedure and are able to return to their normal pre-operative activities. As each case is unique, we would recommend speaking with Dr. Albert specifically about his prognosis for your specific procedure.
Am I A Candidate For PLDF?
Dr. Albert’s first treatment options for lower back pain are nonsurgical. These include physical therapy, epidural steroid injections, anti-inflammatory medications, and other treatments. However, if these treatments are not effective, if your symptoms worsen, or if nerves are being impacted to the degree where there is numbness, tingling, and possible leg weakness, PDLF can be the best option for relieving the pain.
Will I Need To Avoid Any Medications Or Foods Before And After This Surgery?
You’ll need to discuss any medications you are taking with Dr. Albert during the lead-up appointments for this surgery. Generally, you’ll need to stop all drugs that thin the blood.
These include:
- Aspirin
- Ibuprofen
- Anti-inflammatories
- Fish oil
- Vitamin E
- Herbal Products
- Blood Thinners
- Wintergreen Snuff
You will also need to stop using nicotine products for 1-2 weeks before surgery and twelve weeks after surgery. Nicotine has been shown to delay bone and wound healing after surgery.
We also recommend that you do not use any anti-inflammatory drugs for 12 weeks after surgery as they too can interfere with fusion he
Should I Quit Smoking Before Spinal Fusion Surgery?
We recommend that patients stop using any nicotine products for at least two weeks prior to the surgery and 12 weeks after surgery. There is an increased risk of delayed wound healing and non-union of fusion if a patient utilized nicotine-containing products during this timeframe.
The PLDF Procedure
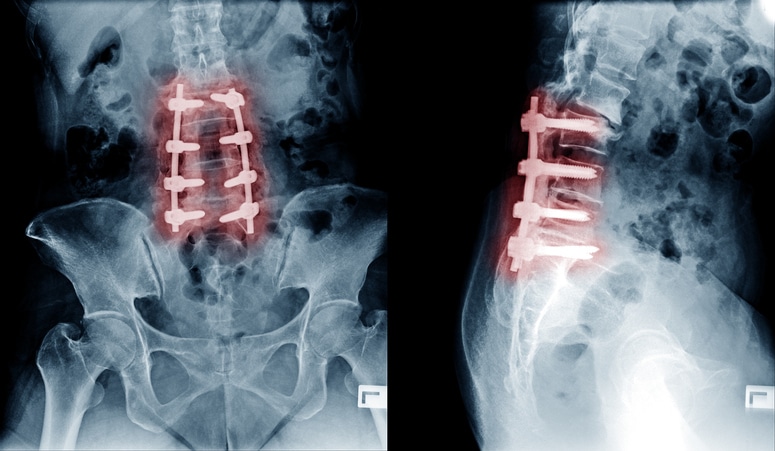
There are two major parts of this spinal fusion. The first being the bony portion of the fusion. This consists of a combination of bone from the bone bank and local bone from the area of the spinal decompression. In a majority of cases, Dr. Albert does not take a bone graft from the patient’s iliac crest (hip area), which means you will not have a separate incision. Bone growth is stimulated and then the grafts are put into place. This fuses the vertebrae and stops the painful movement in the area. The second component of the fusion is the instrumentation. The instrumentation may be rods and screws and/or a cage that is placed between the vertebrae.
Recovery From Posterior Lumbar Decompression And Fusion Surgery
During the first 2-3 weeks, your activity is limited to walking and any exercises taught by the home therapist. We encourage you to walk as much as you are comfortable. During this time, you may go up and down stairs with the use of a railing. You may also sleep in a normal bed. You will be able to lift 5 pounds for the first 2-3 weeks.

The first visit to Dr. Alberts is around 3 weeks after surgery. However, if you have any questions or concerns prior to your first post-op visit, please call the office. After speaking with you, if we believe we should see you in the office we will schedule an earlier appointment.
Do I Need To Get My Sutures Removed After Surgery?
Most patients do not have sutures that require removal after a Posterior Lumbar Decompression and Fusion Surgery. There are internal sutures that will dissolve with time. There may also be steri-strips (white pieces of tape) over the incision that will either fall off or we will remove them during your visit.
How Long Will I Be Out Of Work After PLDF Surgery?
Patients may return to sedentary and light-duty jobs as early as 2-3 weeks after surgery. Your return to work date will be dependent upon the nature of your work and your recovery after the surgery. Most patients are able to return to work by 4-6 weeks after surgery.
When Will I Be Able To Drive After PLDF Surgery?
Patients may begin driving once you are off narcotic and are able to safely and comfortably drive. This usually occurs sometime between one to two weeks after surgery. This timeframe varies for each patient. When you are first attempting to drive, you should only plan on driving a short distance and you should have another driver with you in the car. Once you have accomplished a short drive without pain, you can move up to longer drives.
Will I Need Physical Therapy After A PLDF Procedure?
You will work with both an occupational therapist and a physical therapist after this surgery. Your physical therapist will get you up and out of bed walking several times a day. This is important for your recovery and to avoid the development of blood clots in your legs.
After your first visit with Dr. Albert, you will be given a prescription to start outpatient physical therapy. Your physical therapy program will likely include exercises to strengthen your back and low-impact aerobics, such as walking or swimming. Your therapist will show you how to make modifications to your daily standing, sitting, and sleeping habits. The goal of your exercises will be to strengthen the muscles that support your lumbar spine.
What Will Life Be Like With The Titanium Instrumentation?
PLDF Surgery Testimonial
"Dr. Albert is without a doubt, the most gifted, competent and skilled spinal surgeon a patient could ask for. He is truly warm, compassionate, responsive to the needs of his patients and very caring. Dr. Albert performed a Lumbar Laminectomy a few months ago, and I am happy that I selected him to perform the procedure. Clearly, I have total confidence and trust in Dr. Albert, and he is a credit to the Hospital for Special Surgery. <br></br> Thank you Dr. Albert!"
"I can honestly say that Dr. Albert is above yelp reviews. He is a top-notch spine surgeon and I attribute getting my life back to him. I had two surgeries with him and I cannot even begin to state how incredibly kind and talented he is. He went above and beyond for me. Most importantly, his skill is unmatchable and his position at the top orthopedic hospital proves so."
Click here to view more patient testimonials.
Is PLDF Surgery Painful?
Please keep in mind that pain is a very subjective experience and one’s reaction to surgery is affected by a variety of factors as mentioned above. It is not uncommon for patients to experience “reminder” pain after surgery. This is when a patient begins to experience the same symptoms as they had before surgery. While this is common in recovery from spine surgery we understand that this can be very concerning to our patients. We encourage you to call the office with any concerns you may have after surgery.
What Kind Of Risks Are Involved With PLDF?
The principal risk for this lumbar fusion surgery is that a solid fusion won’t build between the fused vertebrae. However, fusion success rates for this surgery are high, ranging from 90-95 percent. The odds of an unsuccessful fusion rise with patients who smoke are obese, have had multiple level fusion surgeries, or have been treated with radiation for cancer.
As with any surgery, there are risks of infection and bleeding. These complications are uncommon with this procedure (1-3 percent of cases). There is also the small risk that the fusion won’t alleviate the pain.
Schedule A Consultation
If you are interested in posterior lumbar decompression and fusion surgery and would like to see if you are a good candidate, contact our New York City office at 212-606-1004 or fill out an online contact form and our office will be in touch with you about your back surgery options.