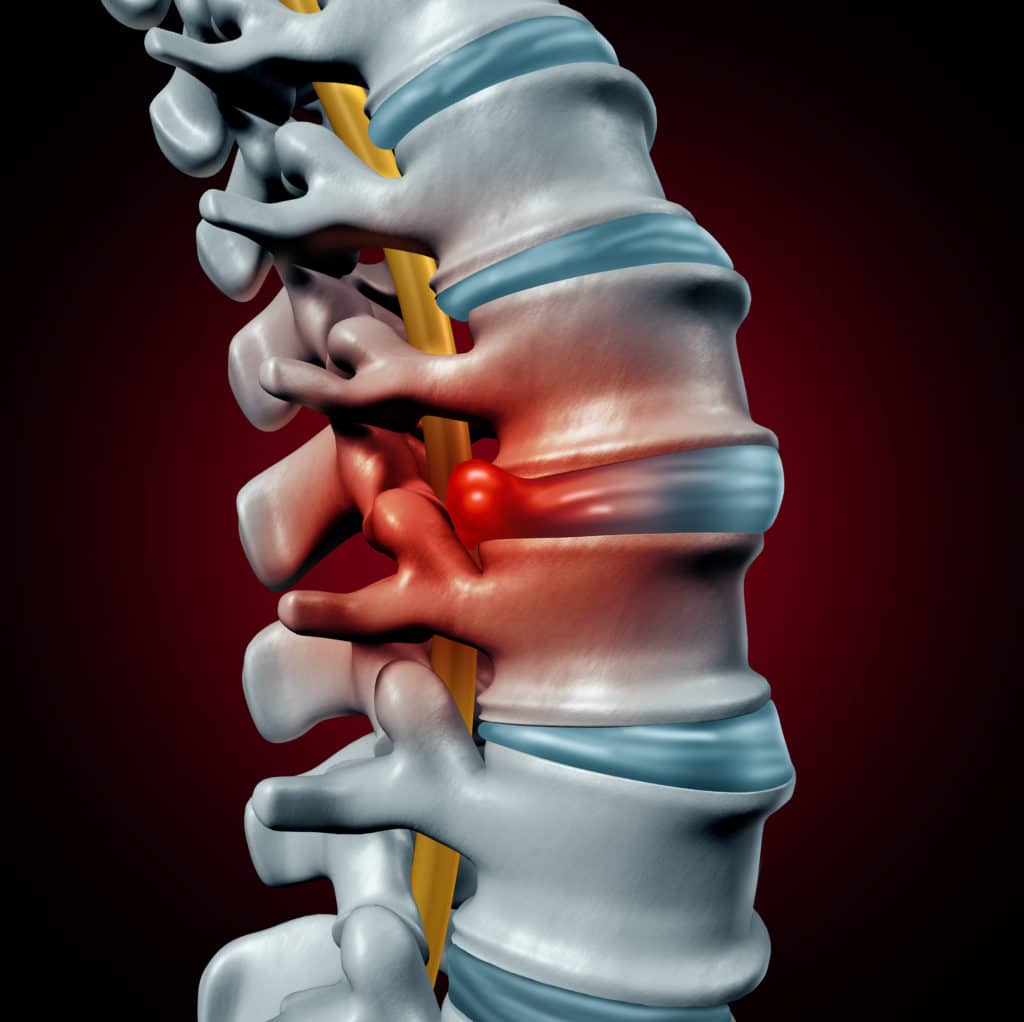
When a patient is experiencing neck and radiating arm pain due to a spinal disc pressing on nerve roots exiting the spine, Dr. Albert may use a cervical posterior foraminotomy to relieve the compression.
Patient Testimonial
"I can honestly say that Dr. Albert is above yelp reviews. He is a top-notch spine surgeon and I attribute getting my life back to him. I had two surgeries with him and I cannot even begin to state how incredibly kind and talented he is. He went above and beyond for me. Most importantly, his skill is unmatchable and his position at the top orthopedic hospital proves so."
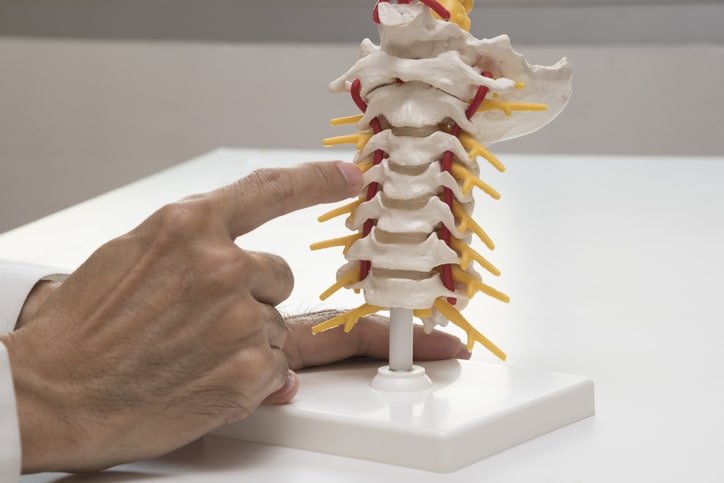
What Is Cervical Posterior Foraminotomy?
The goal of this procedure is to create more space for a compressed spinal nerve in the neck. The procedure relieves the pressure that is being caused by a herniated or bulging disc that is pressing on a nerve root.
The term posterior refers to the procedure being done from the back of the neck. Foraminotomy refers to enlarging the foramen, the opening in the vertebra the nerve passes through as it exits the spine.
How A Cervical Posterior Foraminotomy Helps Treat Chronic Pain
Either the spinal cord or, more commonly, the nerve roots exiting through the foramen of the cervical vertebrae can be affected by the compression. If the patient has degenerative disc disease, the bone itself can begin to wear out and develop bone spurs. These can push on the nerve roots. Otherwise, the usual cause of this compression is the spinal discs. They can weaken and bulge outwards. In more extreme cases, the disc can herniate, allowing the inner gel to push outward and impact the adjacent nerve root.
This pressure on the nerve roots leads to neck pain and pain that can radiate out into the arms and hands. There can be tingling or pins and needles sensations in the arms and hands. This is called radiculopathy.
If not addressed, this nerve compression can lead to permanent nerve damage and impaired function of the hands and fingers.
What Are The Benefits Of A Cervical Posterior Foraminotomy?
This surgery creates more space for the compressed spinal nerve in your neck. It relieves the pressure on the nerve and ends the corresponding pain in the neck, arms, and hands. This procedure has an 85-95 percent success rate in relieving the pain of nerve compression in the neck.
What You Should Know About The Anatomy Of The Spine Related To This Surgery
In the cervical spine, there are seven vertebrae with six intervertebral discs between them. The discs provide cushioning between the vertebrae, and they allow the spine to bend without the vertebrae impacting one another. These spinal discs consist of a tough outer shell called the annulus fibrosus surrounding a soft jelly interior, called the nucleus pulposus.
The annulus distributes the forces placed upon the discs by the vertebrae, while the nucleus provides the cushioning and flexibility.
When we’re young, the nucleus gel is soft and squishy. But as we age, the cervical discs lose water, stiffen, and become less flexible in adjusting to compression. This degeneration can lead to herniation when force is applied to the disc. A disc herniates when the gel pushes through the annulus and presses on a nerve root and/or a spinal nerve. For the cervical spine, these nerves innervate the shoulders, arms, and hands. If the nerve roots are compressed by a herniated or bulging cervical disc this may create pain, weakness or numbness and tingle in the neck and into the arms and hands.
In the vertebrae themselves, there are two structures that come into play with cervical pain. The vertebral foramen houses the spinal cord. Nerves exiting the spinal cord run through the neuroforamen, which are located between adjacent vertebrae. The lamina is a bony protective vertebral arch on the rear/posterior of each vertebra. Both the foramen and the lamina may need to be partially cut away or opened to create room for the compressed spinal cord (lamina) or spinal nerve roots (foramen) to alleviate pain.
Candidacy For A Cervical Posterior Foraminotomy
When a nerve root is compressed in the neck, the symptoms can range from mild neck pain to severe numbness in the hand and electric-like pain shooting down the shoulder, arm, and hand. Depending on the degree of compression, the patient may have significant weakness in the arm or hand.
As with all patients, except in cases of emergency trauma, the last resort for Dr. Albert is surgery. Conservative treatments such as physical therapy or corticosteroid injections are possible alternatives. However, if the pain doesn’t respond to these measures, surgery to relieve pressure on the nerve could be necessary.
Is The Cervical Posterior Foraminotomy Painful?
Spine surgery is not painful. This procedure is performed with general anesthesia, which renders the patient unconscious. In this state, as a result of a precise combination of medications, the body’s pain receptors are shut down. General anesthesia also relaxes muscles and causes an amnesia effect that inhibits memory of the procedure. After surgery, prescription pain medication helps manage comfort through the healing process.
How Long Does The Cervical Posterior Foraminotomy Procedure Take?
The entire operation may take approximately two hours. Patients are escorted to the operating room well before surgery to complete any last-minute preparations. General anesthesia is administered at the onset of surgery and takes only a few minutes to effectively achieve a sleep-like state. Patients are monitored throughout their procedure.
How To Prepare For Surgery
Before your cervical spine procedure, you will receive an outline of preoperative instructions. Patients who smoke are advised to quit as soon as possible. If assistance is needed, the doctor may be able to provide reliable resources to stop smoking. Some patients may need to stop taking certain medications or supplements. For example, blood thinners should be avoided before a surgical procedure to prevent unnecessary bleeding risks and excessive bruising. The doctor may order additional imaging tests or lab work to obtain more information regarding the spine and affected nerves before surgery.
How Is A Cervical Posterior Foraminotomy Done?
To increase the space for the nerve root as it travels through the foramen, Dr. Albert may remove a portion of the foramen, basically enlarging the opening. He also may remove a portion of the lamina, the portion of the vertebra that forms the rear of the spinal canal.
If a herniated disc is pressing on the nerve, Dr. Albert carefully lifts the nerve root and removes the portion of the disc causing the problem.
When the nerve root has ample space, the incision is closed and the procedure is complete.
What Kind Of Results Can I Expect From A Cervical Posterior Foraminotomy?
Most of our patients report significant improvement in their pre-operative pain after surgery. They also report that they are able to return to their normal daily and recreational activities.
Will I Need To Wear A Brace After A Foraminotomy?
Patients typically wear a soft cervical collar, which reduces stress on the neck area and helps decrease pain, in the early postoperative period. This collar is generally worn for two weeks from the date of surgery. The collar may be taken off when eating or showering.
What Kind Of Anesthesia Will Be Used In This Procedure?
This surgery is performed using general anesthesia.
Recovery After A Cervical Posterior Foraminotomy
You’ll spend 1-2 nights in the hospital. During this period physical and occupational therapists will meet with you to instruct you on the proper techniques for walking, getting in and out of bed, and other common movements. You’ll be instructed to avoid excessive bending or twisting of your neck for the first one to two weeks after surgery. Patients can gradually begin to bend and twist their neck after 2-3 weeks, and as pain dictates. Heavy lifting needs to be avoided for the first 4-6 weeks.
Pain varies between patients, but it can be moderate. Dr. Albert will prescribe pain medication for you. Most patients can begin driving in just 1-2 weeks, depending on their level of pain. Patients can return to desk work as early as 1-2 weeks after surgery, again depending on the level of pain. Light recreational sports can resume in as early as one month, with heavy lifting and other sports activities in 1-2 months.
What’s The Difference Between A Foraminotomy And A Laminotomy?
Both of these procedures are decompression procedures. As mentioned above, the lamina bone forms the backside of the spinal canal and makes a roof over the spinal cord to protect it. The intervertebral foramen is the pathway through which the nerve travels as it exits the spine.
A foraminotomy is the removal of bone from within the intervertebral foramen. During the procedure, the bulging or herniated portion of the spinal disc pushing on the nerve root is usually also removed.
A laminotomy is the removal of a small portion of the lamina and the corresponding ligaments, usually on one side. By not removing the full lamina the natural support provided by the lamina is left in place. A laminotomy creates more room for the spinal cord.
A foraminotomy usually deals with compressed nerve roots exiting the spinal cord. A laminotomy usually deals with a narrowed spinal canal or a compressed spinal cord.
The Risks Of A Cervical Posterior Foraminotomy
As noted, this procedure with Dr. Albert is very successful in alleviating the neck and arm pain associated with this type of cervical nerve compression. This is considered to be a low-risk procedure. These are the risks involved: excessive bleeding, infection, reaction to anesthesia, neck stiffness, repeat disc herniation, incomplete relief of the pain, or damage to the nerve root or spinal cord.
How Soon Will I See The Results From My Cervical Posterior Foraminotomy?
Every patient has a unique recovery experience. We expect comfort and range of motion to improve over a 6 to 12 week period. However, within 2 weeks, pain is often improved enough that a patient can return to work and other light activities.
How Long Will The Results From Cervical Posterior Foraminotomy Last?
Numerous research studies have been performed to assess the success rate of cervical posterior foraminotomy. Medical journals indicate that good or excellent outcomes are achieved in 84% to 95% of cases. Patients experience the rapid and lasting improvement of radicular arm pain and can resume most of their normal activities.
Schedule A Consultation
If you would like to learn more about the Orthopedic services that Dr. Albert offers, call our office at 212-606-1004 and schedule a consultation. Dr. Albert proudly serves patients from Manhattan and surrounding areas in New York.