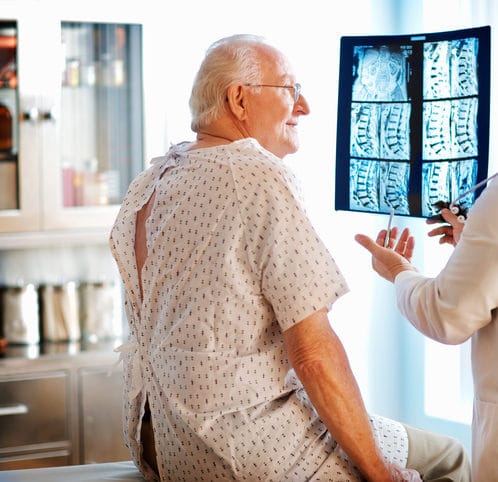
Todd J. Albert, MD is a leading expert in all spinal care and is exceptionally qualified in herniated discs. His practice’s main goal is to provide care and treatment for anyone suffering from spinal related issues.
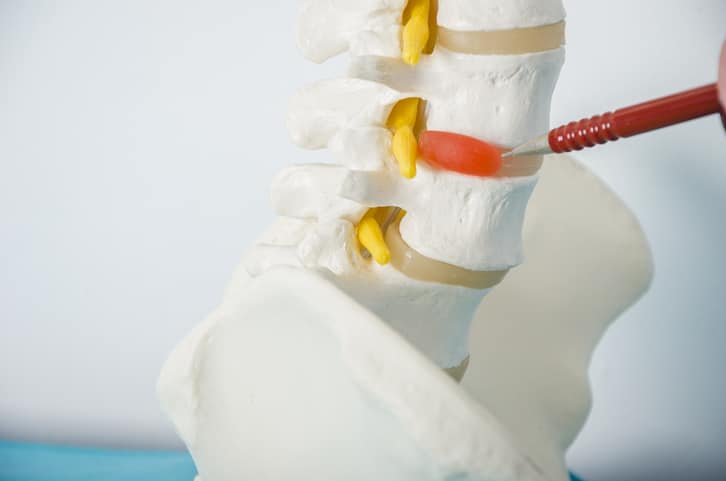
What Is An Intervertebral Disc?
The spine is made up of numerous bones called vertebrae. Discs are donut-shaped structures situated between each pair of vertebrae. Discs have a gel-like nucleus surrounded by strong capsules that hold the liquid center in place. Discs serve as:
- Shock absorbers to prevent friction between the bones of the spine
- Stabilizers that hold the bones of the spine in place
- Cartilaginous joint structures that allow the spine to flex
What Is A Herniated Disc?
The gelatinous center of each spinal disc should remain fully contained within the outer layers of the disc. Injury or degeneration in the spine can cause the jelly-like substance within the disc to migrate outward. A herniated disc is an example of what is called a sequestration injury. It involves the leakage and separation of the nucleus from a disc. The soft disc matter can then press on a nearby nerve root, causing symptoms.
What Causes A Herniated Disc?
The most common factor leading to a herniated disc is age-related degeneration or the wear and tear on the spine that occurs over time. With age, the discs in the spine may become relatively dehydrated. This dehydration decreases their flexibility and increases the risk of tear or rupture during seemingly minor physical movements. In many cases, no cause can be pinpointed for a herniated disc.
What Are The Symptoms Of A Herniated Disc?
Some people go months or years with a herniated disc and experience no symptoms. It is when the gelatinous substance from the disc comes into contact with a spinal nerve root that symptoms occur. These may include pain, tingling, numbness, or an electrical sensation around the spine or down the arms or legs, depending on where the herniation has occurred. Symptoms usually occur only on one side of the body.
Severe herniation can lead to pain or numbness in the perineum or loss of bladder or bowel control. These symptoms indicate a potentially serious condition and need to be addressed right away.
How Is A Herniated Disc Diagnosed?
The initial phase of treatment involves a thorough consultation and examination in our office. A complete medical history and recollection of a known injury can help your doctor identify the source of pain. In addition to the consultation and examination aspect of care, certain imaging tests may be ordered. MRI, or magnetic resonance imaging, is a non-invasive test that enables us to observe soft tissues including the intervertebral discs.
What Are The Benefits Of Herniated Disc Surgery?
The benefits of surgery for a herniated disc are many, however, the main goals are pain relief and prevention of symptom progression. Statistics show that 95% of people who undergo surgery for a herniated disc experience noticeable relief of their symptoms.
What Surgical Treatments Are Available For A Herniated Disc?
Several techniques have been developed to treat herniated discs. These include:
Laminoplasty
The laminoplasty, a restorative spine surgery, can be performed on any of the three spinal segments. The procedure involves opening the lamina, the small section of bone at the back of the spinal cord, and insertion of titanium wires and spacers to reduce nerve compression.
Discectomy
Herniated discs in the low back, or lumbar spine, may be repaired with microdiscectomy surgery. During this procedure, the herniated disc itself is modified to release pressure on the nerve root.
Arthroplasty
Cervical discs that have been damaged may be treated with arthroplasty, a procedure in which the natural disc is completely replaced with an artificial disc. The objective of cervical arthroplasty is to reduce nerve pressure while preserving mobility in the neck.
Spinal Fusion
This surgical technique is may be performed on the cervical or the lumbar spine. The procedure fuses bones together as needed to stabilize a spinal segment that has become compromised by degeneration or injury.
Patient Testimonials
"He is an excellent surgeon and a kind, compassionate man. I had a previous fusion (by another surgeon) and needed another level fused after 7 years. He determined the best way to deal with this and did a great job. His staff is also great to deal with."
"Dr. Albert and his staff provide an extremely high level of care. He is the consummate professional in his area of expertise. Not only is he an excellent doctor, but he is also a very well-rounded human being. As a patient, I feel both confident in his surgical abilities and his personal caring approach to my surgical needs. I have recommended him to a number of my friends and coworkers."
What Are The Risks Of Herniated Disc Surgery?
It is important to note that all surgery does carry some risk. General surgical complications include infection, bleeding, blood clots, and anesthesia reactions. There is a risk of nerve damage associated with any spinal surgery due to the proximity of nerve roots to the vertebra and spinal canal. Damage to nerves in the operative area can lead to prolonged numbness or changes in sensation. The most common nerve damage associated with a herniated disc is caused by the compression related to the herniated disc itself before it is surgically repaired. When the nerve is too extensively damaged by compression, it may take longer to recover after surgical decompression.
Spine surgeries have become much more conservative and safe over time, however, all surgical procedures carry risks that include:
- Anesthesia reaction
- Infection
- Bleeding
- Blood clots
- Nerve damage
- Re-injury of the disc after surgery

How Long Is The Recovery Process For Herniated Disc Surgery?
Herniated disc recovery may vary based on the location of the slipped disc and the procedure performed. Most back surgeries for herniated disc repair require a two-week period of rest and limited activity followed by rehabilitation with physical therapy.
Herniated Disc Surgery FAQs
Can Disc Degeneration Be Hereditary?
Yes, there are studies that suggest that a person with a family history of degenerative disc disease may have a greater risk of developing this same problem. Lifestyle habits like smoking and having poor posture may also present a risk for spinal problems. Larger bodies of research indicate that the natural aging process is the primary factor in degenerative disc disease.
Can You Become Paralyzed From A Herniated Disc?
Paralysis, although extremely rare, is a potential complication of a severely herniated disc. This complication can often be prevented with prompt consultation and treatment.
How Long After My Herniated Disc Surgery Can I Drive Again?
Recovery time and activity restrictions may vary slightly from one person to another. Generally, patients are advised not to drive for at least 1- 2 weeks after lumbar discectomy surgery. During the course of recovery, Dr. Albert will conduct a follow-up visit to check on your progress and recovery. As a sensation, range of motion and comfort improve, activity restrictions are gradually lifted.
Can A Chiropractor Heal A Herniated Disc?
Herniated discs are interesting. They can go unnoticed for months or even years before exhibiting symptoms such as pain, tingling, numbness, or other sensations. When symptoms do develop, it is important to consult with a spine specialist. This specialist could be a chiropractor or an orthopedist. It is important that whomever you see orders x-rays and perform a thorough neurological examination before any treatment is administered. Ideally, people who are experiencing persistent or recurring back pain should schedule a consultation and examination with a spinal surgeon. Having a consultation with a spine surgeon does not mean that you will automatically be referred for surgery and it is often quite the opposite.
Although a spinal surgeon specializes in surgical interventions, we also believe that conservative treatments should be exhausted first before recommending surgery. These conservative treatments may include chiropractic care, physical therapy, or injections. These recommendations are subjective from patient to patient and dependent upon your unique situation.
How Can I Prevent Reinjuring My Disc?
The following suggestions may help patients avoid new or recurrent herniated discs:
- Learning to manage stress, which is often held in the area around the spine.
- Learning and practicing good posture and body mechanics when lifting objects and engaging in physical activity.
- Strengthening the core muscles around the midsection. After surgery for a herniated disc, our patients have prescribed a course of physical therapy that will teach them how to do this with patient-specific exercises.
- Maintaining a healthy weight to prevent excess physical stress on the back.
Schedule An Appointment
If you are experiencing a herniated disc, call 212-606-1004 or fill out our online form to schedule a consultation with New York Spine Surgeon, Dr. Todd J. Albert.