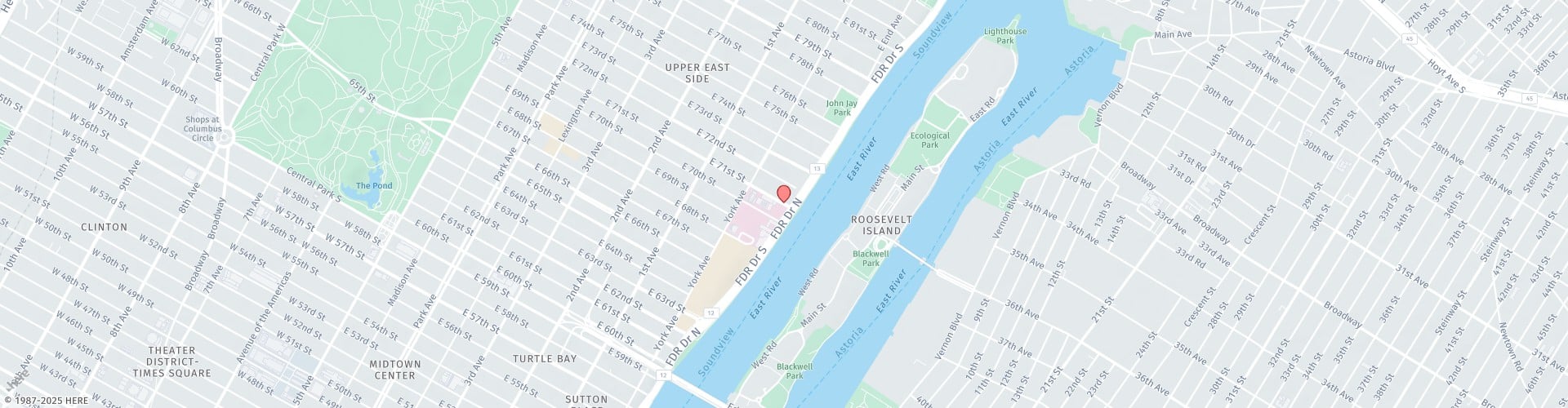
What Is The Lumbar Spine?
The lumbar spine refers to the lower area of the spine between the pelvis and thoracic cage. It is made up of 5 vertebrae (although some people may have 6) that are stacked on top of each other with cushion-like intervertebral discs in between. The lower back is the largest movable segment of the vertebral column and is extremely vulnerable to disorders, making it the source of many pain complaints.

Symptoms Of Lumbar Spinal Issues
The different kinds of back pain are universal up and down the spine. The lumbar spine, however, is the area of the spine that is most prone to injury or the effects of aging, which shows itself in acute or chronic pain.
These are typical symptoms:
- Persistent aching or stiffness
- Sharp, localized pain (usually after lifting heavy objects or overuse)
- Chronic ache, especially after sitting or standing for long periods
- Back pain that radiates down into the buttock, the back of the thigh, the calf, and the toes
- Muscle spasms when trying to straighten the spine
Causes Of Lumbar Spine Pain
Pain in the lower back/lumbar spine can originate in the nerve roots exiting the spine, the joints, the discs, the vertebrae, and the muscles. Many times pain will be a result of a combination of factors from different areas, such as when degenerating discs allow for nerve compression.
These are some of the more common causes behind your lower back pain.
- Degenerated discs — The disc between your vertebrae act as shock absorbers and cushions, enabling movement. They are made of a tough outer shell and an inner soft gel. As we age, the discs harden and thin, and this can lead to pain in the disc space.
- Lumbar disc herniation — Due to the forces impacting the lumbar spine, the discs in this part of the spine are under the more pressure. As we age, our discs harden and become less malleable. Force applied due to heavy lifting or from continued wear can cause a disc to herniate, where the outer shell tears and the inner gel pushes outward. This gel can then push on a nerve root, leading to pain.
- Osteoarthritis — This type of “wear and tear” arthritis can cause the cartilage covering the facet joints in the back of the spine to wear. This can produce bone spurs and swelling in the joint. Bone spurs often result in compression of the nerve roots exiting the spine, causing chronic pain.
- Muscular problems — Muscle strains are the most common cause of lower back pain. Heavy lifting, bending, twisting, or heavy repetitive use can strain these muscles. Unlike most of the pain caused by compression and herniation, muscle strains in the back can cause severe pain. Fortunately, they will heal on their own in days or at most a few weeks.
- Lumbar stenosis —Development of degenerative changes in the intervertebral discs and the joints can create a narrowing of the spinal canal. This tightening can create pressure on the spinal cord, which may then lead to issues with movement and coordination in the arms and legs.
- Lumbar Spondylolisthesis — When one vertebra moves forward over the one below it, this is called spondylolisthesis, and it can lead to nerve compression that causes pain in the legs and feet. This is most common in the lower lumbar spine, L4-L5 or L5-S1.
- Sacroiliac joint dysfunction — This joint, where the spine connects to the top of the tailbone, can be a source of compression and pain, which usually radiates into the legs.
- Lumbar Radiculopathy – This disease involves the compression of the lumbar spinal nerve root. This can cause pain, numbness, or weakness to the areas of the buttock and leg.
Are There Things I Can Do To Prevent Lumbar Spine Pain?
While exercise is important for overall health, the wrong sort of exercise, such as high-impact exercise, can actually lead to back pain. Low-impact exercise, such as swimming or bicycling, can improve your overall fitness without risking back pain. Dr. Albert would recommend meeting with a physical therapist who can provide direction of strengthening exercises for your abdominal and lumbar muscles, as well as teach you proper mechanics for bending, lifting and twisting.
What Is Lumbar Spine Surgery?
Dr. Todd Albert may recommend surgery to address a patient’s pain if the pain does not respond to nonsurgical treatments. Surgery is usually not considered immediately, except in the case of severe trauma, but is usually an option after 6-12 weeks of other nonsurgical treatments. Spinal surgery is usually not recommended for mild to moderate lower back pain.
However, if the patient has disc herniation or nerve compression from bone spurs or spinal stenosis, these conditions will likely not improve without surgery.
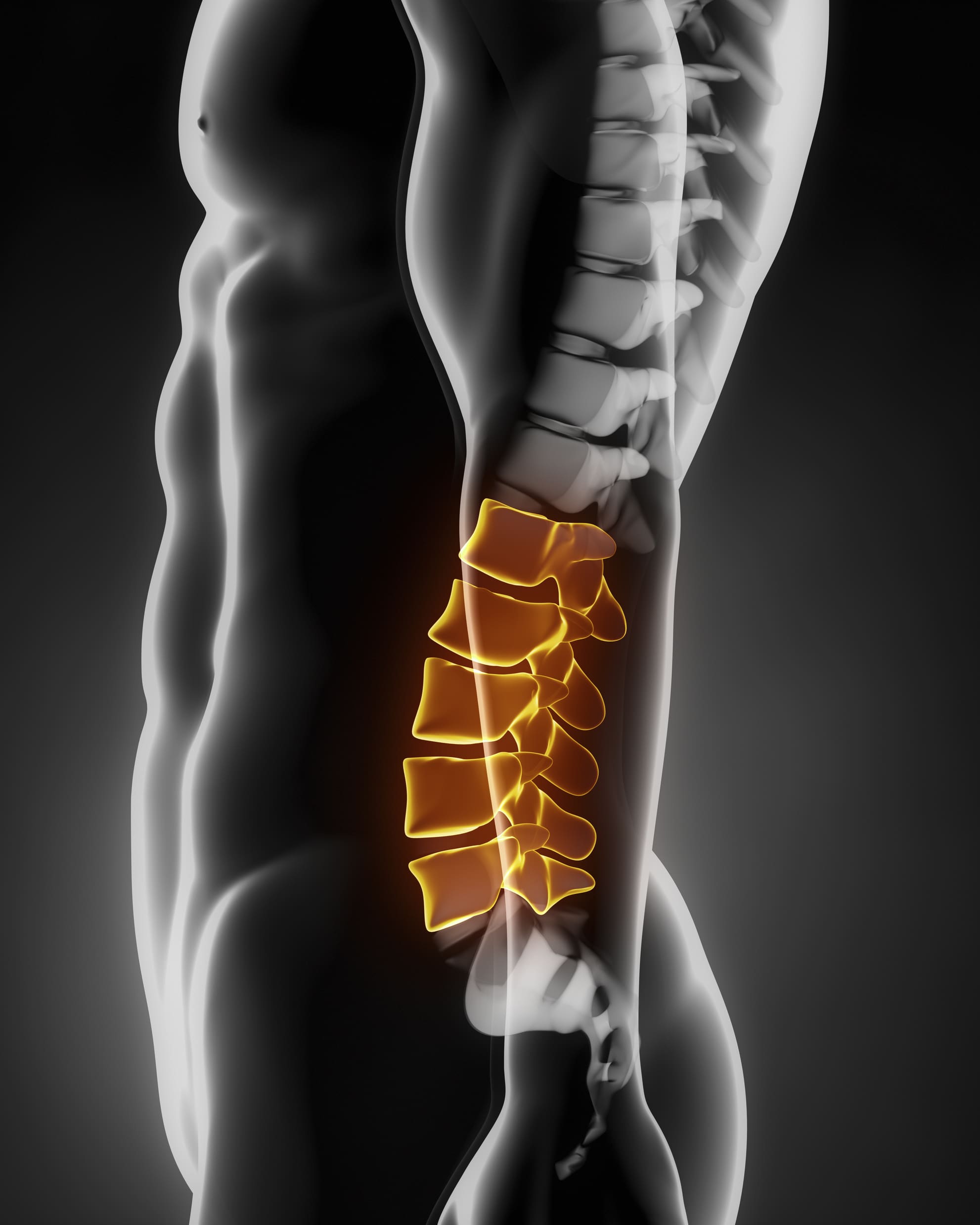
There are two general types of lumbar spine surgery that either aim to decompress the nerve root that is being pinched, or to limit the motion between two or more vertebrae in the lumbar spine that is causing pain.
Here are the procedures Dr. Albert performs on the lumbar spine, with brief descriptions of each. For more detailed information, you can link to each individual procedure page.
Benefits And Risks Of Lumbar Spine Surgery
Spine surgery has evolved significantly over the last 15 years. Today, many spinal procedures are performed using minimally invasive techniques that shorten recovery time without diminishing the results that can be achieved. Minimally invasive spine surgery is performed with very small incisions, often less than one inch in length, and endoscopic instruments like tiny cameras. Most procedures performed today are much better at reducing blood loss and damage to blood vessels, nerves, and muscles. The result of this evolution is less time in the hospital and a more comfortable recovery period.
As much as surgical procedures and techniques have improved, all surgeries carry some risks. The primary risks include bleeding and infection, both of which are minimized with shorter incisions. Spinal surgery also carries risks of nerve damage, an uncommon complication that occurs in a very low percentage of cases.
What Is The Success Rate For Lumbar Spine Surgery?
The success of spinal surgery depends on a variety of factors. These may include the type of procedure performed, the extensiveness of the procedure (how many levels of the spine are treated), the patient’s age and general health, and the source of pain. According to many years of research, spine surgery for leg and lower back pain has a success rate of 70 to 90 percent.

Most patients experience a satisfactory degree of improvement in comfort and range of motion, if not complete relief from their symptoms.
Even when surgery does not fully eliminate pain, patients often describe their results as life-changing do to their ability to engage more in their lives.
Recovery can vary for every patient. It is important to go into spinal surgery understanding that your healing may differ from anyone else’s. It can take anywhere from a few weeks to a few months to begin feeling a positive difference in comfort after a spinal procedure. In some cases, a second surgery is needed. This isn’t because the first procedure failed. In many cases, the second procedure is necessary to address a different part of the spine that is involved in pain.
How Long Will The Procedure Take?
The duration of a spinal procedure can vary based on the particulars of the case. Some patients’ procedures take only 2 hours, while others may take nearly 7 hours to complete.
Surgical time is dependent on the extensiveness of the procedure, how much nerve decompression is needed, and other factors. Before surgery, patients can expect their surgical team to provide them and their families with an estimated surgery time. Often, the surgical team also checks in with the family to keep them informed of the progress of the procedure.
Candidates For Lumbar Spine Surgery

The decision to proceed with surgery is a difficult one and is generally up to the patient, based on their individual level of pain and dysfunction. Dr. Albert often recommends that you first attempt to treat the pain related to your spinal problem with conservative treatments such as physical therapy or injections.
However, if your pain doesn’t respond to nonsurgical treatments, surgery may be the only long-term solution to gain relief of the symptoms. Nerve compression, spondylolisthesis and stenosis do not resolve on their own without intervention.
Types Of Lumbar Surgery
Dr. Albert offers different options for lumbar spinal surgery. During your consultation, we will figure out which option is best for you. The types of surgery Dr. Albert offers include the following:
Lumbar Laminectomy Surgery (PLD)
A lumbar laminectomy (PLD) is performed to relieve pressure on the spinal cord or nerves. The surgery removes a portion of the herniated disc that is pressing on the nerve. This helps relieve the pain and protect against permanent nerve damage.
Microdiscectomy
Microdiscectomy is one of the most common spine surgery procedures. This surgery relieves pressure on the nerve and removes the source of the pain.
Posterior Lumbar Decompression And Fusion (PLDF)
Posterior lumbar decompression and fusion (PLDF) is a surgical procedure that aims to relieve pain and pressure on the spinal cord and the nerves in the lower back.
Transforaminal Lumbar Interbody Fusion (TLIF)
Transforaminal lumbar interbody fusion (TLIF) is a procedure that fuses the anterior and posterior columns of the spine through a posterior approach. This approach results in less disturbance to the nerve roots, reducing the risk of scarring or injury to them.
Patient Testimonial
"Great surgeon and did a great job with me. I had several opinions all by top providers and his assessment was the most clear, and plan felt the most appropriate for my specific situation. Accessible pre and post op. Staff is superb. Surgery went smoothly. Full recovery. I’m a surgeon myself."
How To Prepare For Spine Surgery
Before undergoing spinal surgery, some patients may need to alter medications, supplements, or lifestyle habits. Patients who smoke must stop several weeks before surgery. Smoking should be avoided for several weeks after surgery, as well, to help the body heal properly. During your consultation for spine surgery, disclose to your surgical team any and all medications and supplements you take on a regular basis. You may be advised to alter dosages or stop certain substances that can thin the blood. This is a preventive measure to decrease the risk of excessive bleeding during or after surgery.
In addition to preparing the body for optimal healing, patients can also prepare for lumbar spinal surgery by:
- Purchasing slip-on shoes that are comfortable and safe for short walks.
- Placing important items within reach: It is not possible to bend over after lumbar spine surgery, so place items on a counter or at torso height.
- Purchasing a grabber that can help grasp objects from the floor or lower location: A grabber is ideal for picking up dropped items like socks, and can help prevent the natural inclination to bend over to pick up low-sitting objects.
- Getting a toilet riser: This medical necessity elevates the toilet seat to prevent bending too far at the hips and knees to use the restroom.
- Talking to the surgical team about the procedure: Patients who know what to expect from anesthesia, what happens during surgery, and what to expect afterward tend to be more at ease with their treatment plan.
- Meal prepping ahead of time: After surgery, patients cannot do much standing for at least a few days. Having healthy meals in the refrigerator and freezer can minimize stress and also ensure that the body receives the nutrients needed for healing.
Recovery And Aftercare For Lumbar Spine Surgery
Patients who undergo lumbar spine surgery may experience post-operative weakness, numbness, and pain in the area where nerve compression was addressed. Prescription painkillers should be taken as directed to minimize discomfort. The surgeon may also have additional suggestions such as cold compresses to facilitate an optimal recovery.
The length of recovery after a lumbar spine procedure depends on the extent of repair and type of surgery performed. Post-operative instructions also tend to vary between different procedures. Generally, patients need a few weeks of rest and relative inactivity, with the exception of short walks as tolerated. The bones, nerves, and other structures affected by spine surgery can take several months to heal completely. Activity restrictions typically ease gradually over time, with light activity clearance occurring sometime around 4 to 6 weeks after surgery. Patients whose jobs are strenuous and more physically demanding may need more time off work and other activities, as may older patients and those who require more extensive repairs.
After surgery in the lumbar spine region, a patient may need to wear a back brace when walking and sitting. The surgeon may recommend sitting for no longer than 30 minutes at a time, and sleeping in whatever position is most comfortable. It is necessary to carefully follow the post-operative instructions provided to you based on your case, and to contact our office if questions or concerns arise.
Is Physical Therapy Required After Lumbar Spine Surgery?
Physical therapy is often a post-surgical requirement. Seeing a physical therapist as prescribed can help a patient regain strength in the muscles that support the spine and neck. Physical therapy exercise can also help improve flexibility and range of motion, both of which are needed for an optimal recovery. In addition to strengthening the back muscles that support the spine, physical therapy can also help strengthen the core muscles, also involved in spinal movement. Patients who work through a physical therapy program after lumbar spine surgery may complete body weight exercises, resistance exercises, body ball exercises, biofeedback, ultrasound, and more.
FAQs
What Are the Early Signs That I Might Need Surgery?
You might need lumbar spine surgery if you have ongoing lower back pain that doesn't get better with treatments like physical therapy or medications. Other signs include:
- Pain that spreads down your legs
- Numbness
- Tingling
- Muscle weakness
If you have trouble walking or standing for a long time or lose control of your bladder or bowels, see a doctor immediately. These could be serious symptoms that require surgery.
How Can I Tell If My Back Pain Is from My Lumbar Spine?
Lumbar spine pain usually feels like a deep ache in the lower back, which can spread to the buttocks and legs. This pain is often sharp or shooting and can make your legs tingle. It typically worsens with bending or lifting movements and might feel better when lying down.
What Changes Should I Make to Help My Recovery?
To recover well after lumbar spine surgery, try to keep a healthy weight to reduce stress on the vertebrae. Here are some additional steps you can take:
- Do low-impact exercises like walking or swimming to get stronger and more flexible.
- Avoid heavy lifting and intense exercise at first.
- Use good posture and make ergonomic changes in your daily activities.
- Eat a balanced diet rich in fruits and vegetables and stay hydrated.
Can Elderly Patients Have Lumbar Spine Surgery?
Yes, elderly patients can have lumbar spine surgery. Age alone doesn't prevent them from undergoing an operation. The decision depends on the patient's overall health, the symptoms' severity, and the procedure’s risks and benefits.
Modern techniques and better anesthesia make it safer for older adults. Before recommending surgery, Dr. Albert will evaluate your bone density, heart and lung function, and other health conditions.
What Happens During My First Appointment?
During the initial appointment, Dr. Albert reviews your medical history and current condition. He also examines your spine and may ask you to get X-rays, an MRI, or a CT scan.
The doctor will explain the surgical options, risks, and advantages and create a treatment plan for you. This is a good time to ask questions and share any concerns you have.
How Can I Manage Pain While Waiting for Surgery?
To manage pain while waiting for surgery, you can take over-the-counter medications like acetaminophen or NSAIDs. Physical therapy and gentle exercises can help keep you moving and reduce discomfort. Heat or cold packs can provide temporary relief.
Avoid activities that make symptoms worse and use supportive devices, such as braces or ergonomic chairs. Sometimes, Dr. Albert will prescribe stronger drugs or recommend steroid injections for severe pain.
Why Choose Dr. Todd J. Albert?
When you choose Dr. Todd J. Albert, you’re trusting a world-renowned expert in orthopaedic spinal surgery. He is the Surgeon-in-Chief Emeritus at the Hospital for Special Surgery and a Professor of Orthopaedic Surgery at Weill Cornell Medical College. He has been recognized as a top doctor in New York since 2014.
Dr. Albert received the prestigious Nicolas Andry Award in 2019 for his extensive scientific research and advancements in orthopaedic spine procedures. His experience and dedication make him a top choice for patients needing high-quality, compassionate care.
Schedule A Consultation
If you would like to learn more about lumbar back surgery, call 212-606-1004 to schedule an evaluation with New York Spine Surgeon, Dr. Todd J. Albert. You can also go to our contact page to send us an appointment request form, and our staff will help you set up your consult. Our practice looks forward to serving you!